Breast reconstruction can be performed for women who have lost one or both breasts to mastectomy or for women who lack breasts due to congenital or developmental abnormalities. The goal of breast reconstruction is to create a breast and nipple that resemble the natural breast as closely as possible in shape, size and position. A long as a woman is healthy, age is not a factor in whether she is a good candidate for breast reconstruction. However, women with health problems such as obesity and those who actively smoke, are advised to wait rather than have breast reconstruction immediately following mastectomy.
Types Of Breast Reconstruction
Breast reconstruction is performed in several steps and there are essentially two types: autologous and implant based. The type of breast reconstruction used depends on many factors. This decision should be made after a careful consultation and thorough discussion with your plastic surgeon.
Autologous-Tissue Breast Reconstruction
Autologous-tissue breast reconstruction is generally used if there is not enough tissue left post-mastectomy to create a new breast, the remaining tissue has been radiated, implant reconstruction has failed, or if a woman does not want implants. During autologous-tissue breast reconstruction, a breast is created using skin, fat and, sometimes, muscle from other parts of the body. The abdomen, back, buttocks or thighs are all donor sites. The donor tissue, which is called a "flap," is either surgically removed and reattached (free flap) to the chest, or left connected to its original blood supply and "tunneled" through the body to the chest (pedicled flap). There are a number of different flap techniques; which one is used depends on the individual patient. Factors taken into consideration include how much extra tissue is available for transfer; the width and flexibility of blood vessels; and how large the breast(s) needs to be.
Implants may or may not be used with autologous-tissue breast reconstruction. Constructing a nipple and areola is generally performed in a separate surgery.
Oncoplastic Breast Reconstruction
Oncoplastic breast reconstruction is generally used for partial or segmental defects, which occur as a result of a lumpectomy. Plastic surgery techniques and principles utilized in breast reduction surgery and mastopexy allow for simultaneous reconstruction and restoration of breast cosmesis.
Nipple And Areolar Reconstruction
Nipple areolar reconstruction involves creating a new nipple (central projecting portion) and areola (darker outer circle). Nipple areolar reconstruction is generally performed as the final stage of breast reconstruction after the breast mound has been reconstructed and had time to heal. The nipple can be surgically reconstructed using the surrounding skin, which can be elevated and shaped to create true projection.
Traditional tattooing is performed afterwards to provide the appropriate areolar coloring.
Other surgical options include nipple sharing from the opposite breast (if sufficient tissue is present) and skin grafting.
Modern 3D tattoos can also be used to create a realistic appearing nipple and areola which simulate projection and possess remarkably accurate color variation.
Implant/Tissue-Expansion Breast Reconstruction
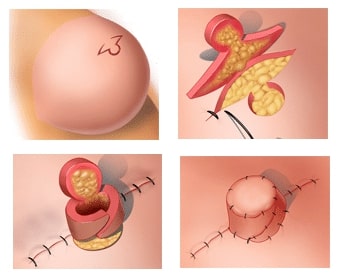
Implant/tissue-expansion breast reconstruction involves inserting an implant in the chest after the skin has been stretched enough by an expander to contain it. First, the surgeon inserts a balloon expander beneath the skin and chest muscle where the reconstructed breast will be built. Then, during the next few weeks to months, a saline solution is injected through a tiny valve beneath the skin into the expander. As the expander fills with saline, it stretches the skin and creates a pocket for the permanent implant. The expander is later replaced with permanent implant, which can be filled with silicone gel or saline. A final procedure reconstructs the areola and nipple. Some patients do not require tissue expansion, which can take up to a year to complete, and can begin reconstruction with insertion of the permanent implant.
It is essential that a patient have reasonable expectations about the results reconstruction provides. During your consultation with your plastic surgeon these expectations should be brought forward and your goals discussed in detail.
Recovery From Breast Reconstruction
Recovery varies widely based upon the type of procedure used for breast reconstruction, as well as whether reconstruction immediately follows mastectomy or occurs in a delayed fashion. Implant based breast reconstruction usually proceeds as day surgery with patients going home the same day after their surgery. Autologous, free flap breast reconstruction requires a hospital stay of 3 to 5 days.
Patients are tired and sore for 1 to 2 weeks and possibly longer depending on the type of reconstruction they have had. Many can return to work within 1 to 2 weeks provided they are not lifting greater than 5 pounds. Recovery can take 3 to 6 weeks depending on the type of reconstruction the patient has had. Exercise and other strenuous activity should be avoided for at least one month.
Compression garments are typically worn if the free flap has been taken from the abdomen (DIEP flap). Sutures do not need to be removed and dissolve on their own over the course of weeks to months. Drains may be left in place to prevent a buildup of fluid in the reconstructed breast or in the abdomen. Drains should be removed based on the volume of drain output and after follow up and discussion with your plastic surgeon; this usually takes 1 to 2 weeks.
Postoperative pain, swelling and sensitivity diminish during the first few weeks. Scars begin to fade within the first months and continue to improve and become less conspicuous over time. Scars can take 1 to 2 years to mature to their final appearance.
Risks Of Breast Reconstruction
In addition to the risks associated with surgery and anesthesia, those related to implant/tissue-expansion breast reconstruction include infection around the implant, implant leaks and ruptures, and implant deflation or shifting. Risks related to autologous breast reconstruction, depending upon the technique used, include fat necrosis, abdominal weakness, bulging and true hernias.
Correcting reconstructive problems typically requires additional surgery.
Results Of Breast Reconstruction
A reconstructed breast will not look the same as the original breast. Although a surgeon attempts to match the size, shape, position and other attributes of the remaining breast, an exact match is usually not possible. To achieve symmetry, the remaining breast may be operated on to make it bigger (augmentation) or smaller (reduction), or to lift it (mastopexy).
In addition to not looking the same as the original, a reconstructed breast has little sensation, although there may be more when autologous tissue is used as compared to an implant.
